Featured Image: totajla on Shutterstock
I was born and raised in rural New South Wales and Queensland. I had heard the word ‘remote nursing’ but truly had no concept until I landed in remote locations in Western Australia (WA).
Having worked my entire career (nearly 30 years) in tertiary hospitals, ‘going remote’ was my adventure. An intensive care unit (ICU) nurse, facing 50, single and with adult children meant I could travel in a different way, jumping in the deep end without any idea what to expect.
For those not familiar with WA, our only tertiary hospitals are in Perth and each region, of which there are seven, has a regional hospital most of which have less than 50 beds. I worked as the Director of Nursing in three very remote hospitals in the Kimberley and Goldfields regions.
Getting out of the car in the Goldfields region of WA, my first thought was ‘there is not enough water here’! The hospital is in a very small, very remote community in the desert, with;
- annual rainfall less than 300ml;
- population less than 1000,
- nearly 1000km from Perth; and
- nearly 300km from the regional hospital in Kalgoorlie.
The remote hospital in the Kimberley is located at the opposite end of the desert to the Goldfields, with;
- population less than 1500;
- nearly 3000km from Perth; and
- 400km from the next closest hospital in Kununurra, with the regional centre in Broome nearly 700km away.
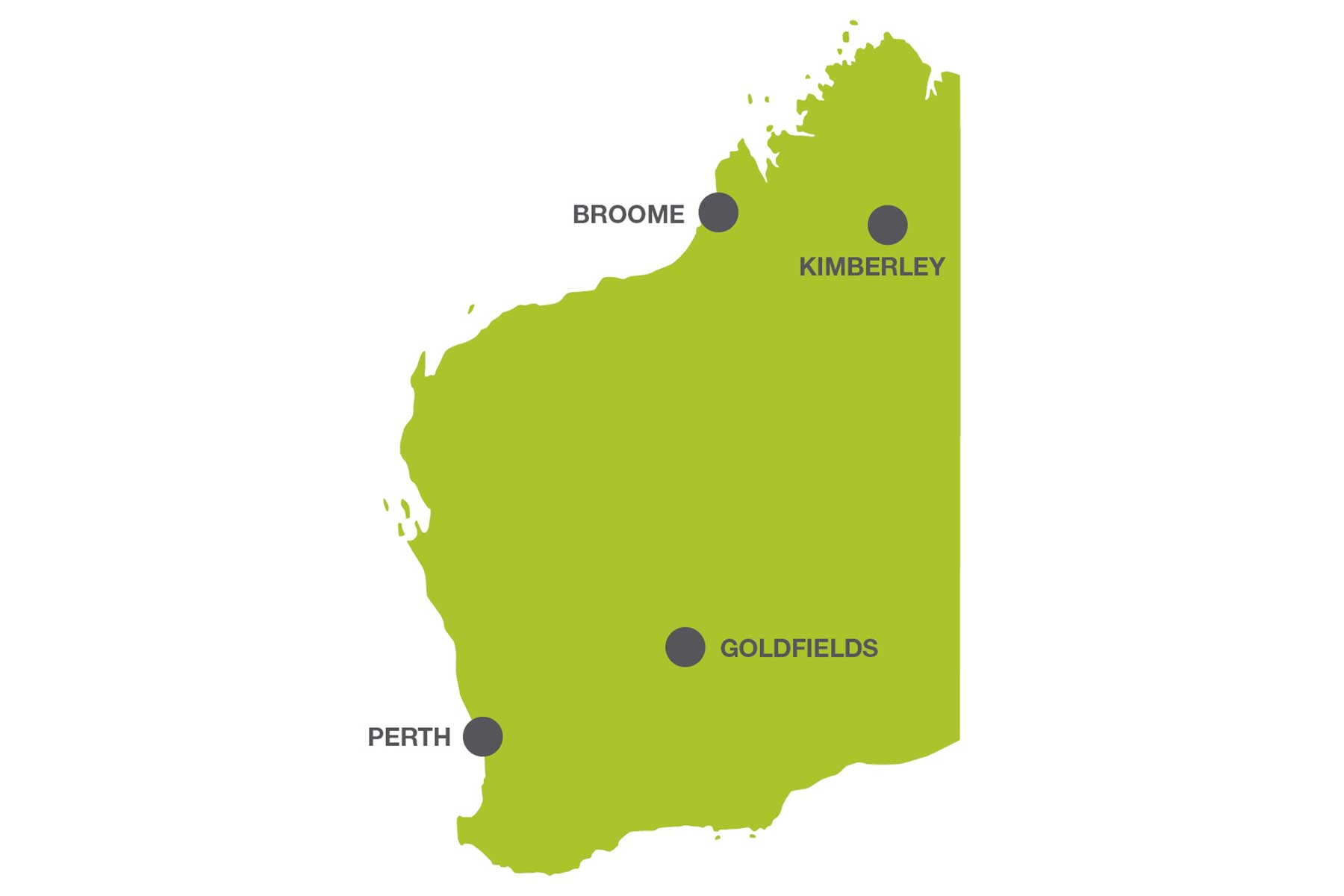
Even these figures mean very little until you arrive, the distances on the page do not do the actual isolation justice.
All three of these hospitals, like over 60 hospitals in WA, have a small emergency department and inpatient beds, with over 40 having aged care residential beds as well. The Goldfields hospital has one doctor most of the year but goes without for long stretches of many weeks. Some of our towns do not have a doctor at all and we rely heavily on an Emergency Telehealth Service for senior medical support.
Remote nursing practice and social life are very different to the norm and I have heard some very interesting comments and questions during my time across the state. You live on hospital grounds or within walking distance; there is always a supermarket with the necessities but do not expect the variety of products that you get from home; and expect to pay a bit more. A lot of towns do not have a café, so take your plunger or coffee machine; and take something to do. You will need to be with Telstra as there is no coverage otherwise – this was a key for staff coming to town as you cannot call if you get lost and neither can you tell your family you have arrived!
The nurses’ scope of practice is so different to when you work in a large hospital, where there is a multidisciplinary team and plenty of you. In very remote hospitals you will learn to be the physiotherapist, the social worker, the phlebotomist, the drug and alcohol councillor, the chronic diseases nurse, the mental health nurse, a paediatric nurse, the wound care nurse, and an emergency department (ED) nurse.
If you come from ED in a large hospital and are used to a large team of people helping you in a crisis, you will learn flexibility and adaptability to manage a crisis with two or three of you and hopefully a doctor alongside you. A patient escort on an interhospital transfer by road could take you six or eight hours. And you may look after a critically ill patient for an extended period waiting for the Royal Flying Doctors. Depending on where you go, nurses learn to run the ambulance service, be the x-ray operator and suture. Your scope of practice is what you make it out there.
For nurses wanting an adventure or something a bit different there is so much to know and learn, different diseases and a different way of working! Whether you are in your early or later career be prepared to be challenged and stretched. You will meet amazingly resilient people in the context of the staff and the community; you will change your expectations of standards of care because it is not the same out there. Everyone has a role to play, and you will find yourself guiding your cook, all purpose orderly or patient care assistant to assist you in a procedure or to get equipment.
Despite the isolation, the comradery you feel in working in these small teams and supporting each other to care for the community (not just individuals) is amazing. No matter what you thought it was going to be like, it will be different. You will learn so much about your nursing practice and capability, you will grow professionally and personally, and you will be forever changed by the experience and by the people you meet.
Kerry Wilcox MACN
Kerry Wilcox MACN has over 30 years of nursing and management experience across metropolitan, regional and remote health systems. Her experience includes Intensive Care nursing, St John Ambulance service, hospital commissioning, public-private partnership, public and corporate sectors, and Department of Health and she has specialities in Clinical Governance and Safety and Quality, innovation and change management, emergency management, and COVID planning and response. Kerry is currently the Operations Manager for the Comprehensive Cancer Centre at Sir Charles Gairdner Hospital and Vice Chair on the 4LifeSkills Board of Directors.






